If new lower limits affect your hypertension status, here's what to do.
By Lisa Esposito|Nov. 17, 2017By Lisa Esposito|Nov. 17, 2017, at 12:49 p.m.High Blood Pressure Guidelines Just Got Stricter
MoreIf you feel like you're doing OK with a borderline blood pressure of 130/80 or so, this is your wake-up call: According to guidelines released Monday, the lower limits of high blood pressure have changed. What counted last week as "prehypertension" is now upgraded to Stage 1 hypertension. So, you've officially joined the ranks of people with high blood pressure.
[See: 10 Seemingly Innocent Symptoms You Shouldn't Ignore.]
Knowledge is power, so use the new designation as motivation to make lifestyle changes, stay on top of your blood-pressure numbers and work with your health care provider to determine whether you need medication, says Dr. Paul Whelton, a professor of global public health at Tulane University in New Orleans, and chair of the 2017 Hypertension Clinical Practice Guidelines that were announced at the American Heart Association's Scientific Sessions 2017, a major medical meeting.
High blood pressure increases the risk of heart disease, stroke and other medical conditions. By taking above-normal blood pressure more seriously – and sooner – health care providers and patients can do more to lower those risks.
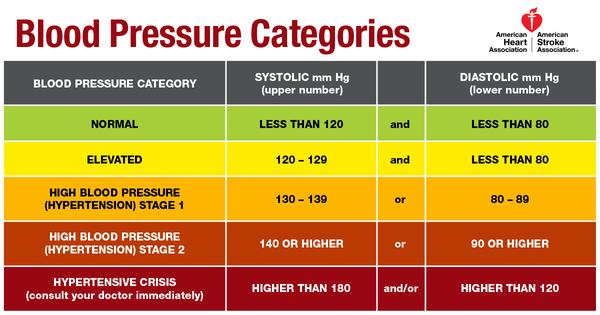
A blood pressure of less than 120/80 is considered optimal for most adults. Before the modification, blood pressure of 140/90 or above was considered hypertension. Now, if your systolic (upper) number ranges from 130 to 139 or your diastolic (lower) number is 80 to 89, that falls under Stage 1 hypertension.
(Nate Hellman)
If you "officially" have hypertension, your blood pressure should be monitored more closely. Your doctor will emphasize the need to make healthy lifestyle changes, such as losing weight, eating less salt, drinking in moderation or not at all and exercising.
Earlier treatment with antihypertensive drugs will be advised for some people due to the updated guidelines, jointly released by the American College of Cardiology and the American Heart Association and published online in their respective journals. However, the increase in people who start on blood-pressure medications based on changed recommendations will be less than 2 percent of those who fall into the new category, Whelton says.
"We like to think, No. 1, that these new guidelines and new classifications will do a better job of alerting people to the need to be attentive," Whelton says. "And, No. 2, determine who will benefit and will need an antihypertensive drug in addition to lifestyle changes."
[See: 15 Best Weight-Loss Diets at a Glance.]
Falling into the new category is concerning, but not a reason to panic. If you think you're affected, take a step-by-step approach.
"First, you obviously want to be sure it's an accurate diagnosis," Whelton says. "So confirming is very important: Making sure that blood-pressure measurements are taken well, taken on more than one occasion and averaged. It's helpful to have out-of-office measurements – we stress that."
The role of patients in monitoring their own blood pressure is much more prominent in the updated recommendations. Checking your blood pressure at home complements the monitoring done by your primary care provider. Home monitoring gives a fuller picture of your blood pressure averages, peaks and lows, rather than relying solely on office-visit checks done at six-month or yearly intervals.
Office and at-home blood pressure readings can differ significantly, says Dr. Wanpen Vongpatanasin, a hypertension specialist and professor of internal medicine at UT Southwestern Medical Center in Dallas. "White-coat hypertension" can occur as patients get nervous when checked by health care providers during office visits, she explains. In contrast, with "masked hypertension," patients may register lower blood pressure at the doctor's office than they routinely experience at home.
Even if you don't have high blood pressure, it's a good idea to check yourself every month or so, Vongpatanasin says. If you are diagnosed with hypertension, particularly if you're starting a new blood-pressure medication, you should check yourself much more frequently – as often as twice daily – to make sure treatment is working. Vongpatanasin offers these tips for getting accurate at-home readings:
Home blood-pressure devices are becoming increasingly user-friendly. Some models sync with your smartphone or computer, which can store your results, average them for more reliability and create easy-to-read graphs. That eliminates the need to manually log results or remember to bring that paper with you for medical appointments.
It could indicate a problem.Allison KleinJune 19, 2017
Several consumer groups have tested a variety of home devices and reported in depth on their pros and cons. Wirecutter recently ranked the Omron Series 10 with Bluetooth as the top monitor for most people to use at home, in terms of accuracy, cuff comfort, user interface and tracking capabilities. It's currently listed at about $62 on Amazon. For those looking for a less-expensive model, the ReliOn BP 200, which retails at Walmart for just under $40, also got good marks for reliability.
[See: 11 Items That Help Protect Your Health.]
Keeping track of your blood pressure is just the beginning. Reversing high blood pressure and maintaining a normal range, ideally through lifestyle changes, is the goal. "It's not easy but it can be done," Whelton says. That includes getting as close as possible to your ideal body weight through physical activity and healthy eating with less salt. He praises the DASH diet, which stands for Dietary Approaches to Stop Hypertension.
If you've just been bumped up to the hypertension status, you're not alone. "With these new guidelines, it is expected that the prevalence of high blood pressure in the United States will increase from 32 percent to 46 percent – almost half of adult Americans will have high blood pressure." Vongpatanasin says.
Your health provider will calculate your cardiovascular risk based on factors including blood pressure, cholesterol levels, sex and age, and medical conditions such as diabetes and kidney disease. If you're considered at higher cardiovascular risk, you'll probably be advised to start treatment, with a single blood-pressure medication or a combination.
Tags: health, patients, patient advice, high blood pressure, heart disease, stroke
Best Heart-Healthy ExercisesWhen to Get a Second OpinionWellness
What Is Poikiloderma?For Better
New Epilepsy Treatment Options